Obesity: A Public Policy Failure
Obesity is the single greatest threat to Americans today. Only thirty years ago, Mississippi topped the rankings with a rate of 15%. In the year 2020, you cannot find a state with less than a quarter of adults suffering from this disease, and Mississippi has climbed to over 40%. We have grown up in an entirely different America than that of our grandparents. Most of us do not remember a United States before the obesity epidemic. Cardiovascular disease is the number one killer on US soil, but a century ago it was almost unheard of. This is not a disease of middle age, either; during the COVID-19 pandemic, we saw the number of children and teens afflicted by obesity rise to almost a quarter. Furthermore, not one country has successfully reversed its obesity epidemic.
It’s easy to think that obesity is simply a product of our modern lifestyle. People just need to eat less and exercise more, right? Everyone “knows” that; however, we do not actually eat or exercise much more or less than our ancestors. We only eat 456 more calories per day on average than in 1970 [2]. Most people work desk jobs, not very physically demanding, but most people worked desk jobs a hundred years ago as well. It’s hard to imagine that 500 calories – the equivalent of a plain bagel with cream cheese – alone has caused an uncontrollable obesity epidemic. In fact, people exercise more than they did ten or twenty years ago, but growth in obesity shows no sign of stopping [3].
In 1971, inmates of Vermont State Prison agreed to volunteer for a study in exchange for shorter sentences: for half a year, researchers consistently overfed them, some as much as 10,000 calories a day [4]. Naturally, every participant added on massive amounts of extra pounds. Most people expect a lifelong struggle of starvation and effort to shed it off, but every single participant returned to normal weight after ten weeks of their usual diets. If our bodies can shed the extra 10,000 daily calories, a mere 500 hardly seems capable of causing a global epidemic. Obesity is categorically different from a simple calorie surplus.
Are carbs and sugar to blame then? Again, Americans have been consuming less sugar and carbs since the turn of the century, with no impact on obesity [5]. By common sense, carbohydrates alone cannot be the cause, because many civilizations since the dawn of agriculture have depended on wheat and rice as staple foods.
“Fat makes you fat” used to be common sense as well. Again, science and statistics paint a different picture. Fat consumption has decreased as obesity spiked and studies cannot find an effect of low-fat diets on body weight [9].
Pre-industrial tribes have eaten incredibly varied diets and have never faced an obesity crisis. The Inuits of the North Pole eat almost exclusively meat and blubber: a diet extremely high in cholesterol and fat [10]. The Kitava tribe of the Pacific subsist on starches from tubers and taro as well as fresh fruit, and they are no more active than any Westerner [8].
By now, it’s clear that the difference between obese and healthy does not come soley from macromolecules, calories, or exercise. These tribes demonstrate that the human body can thrive on an extreme range of diets and macronutrient profiles. The difference stems from pre-industrial to post-industrial.
I argue that some chemical pollutant causes obesity. We know that macromolecules or calories alone cannot account for it. We also know of numerous drugs, such as Clozaril, Zyprexa, Haldol, Risperdal, and lithium, which target the brain and cause massive weight gain in certain patients. Obesity practically did not exist until the middle of the twentieth century, when it began to increase consistently. Current studies say that the vast majority of differences in BMI come from genetics, but a century ago, our genes weren’t any different [14]. More likely, since about sixty years ago everyone in industrialized countries has been regularly exposed to a contaminant that people with certain genomes are more susceptible to.
Antibiotics used in livestock have slowly pervaded through the food chain and into humans. Antibiotics also disrupt the gut microbiome by killing useful bacteria, which affects many aspects of health including BMI and body weight [17]. They also build up in the water supply, which explains the trend in elevation and watersheds, and widespread use of livestock antibiotics began around the middle of the twentieth century [18]. Evidence suggests that vegetarian diets can curb obesity, and one reason for this may be that plant-based diets lack many of the microbiome-killing antibiotics present in non-vegetarian diets [19].
Another candidate is lithium, which most people know as an antidepressant, one of the main side effects of which is weight gain. Lithium production has skyrocketed in recent decades, from virtually none before 1950 to around 25,000 metric tons in 2008 to 85,000 tons in 2018 [21]. States such as West Virginia and Alabama have leading obesity rates which can be explained by lithium runoff from mining. The same trend holds true abroad: high lithium levels in the Caspian Sea and even higher levels in the Dead Sea may be the reason that northern Iran and the West Bank have much higher obesity levels than the surrounding areas [22]. Some of the only countries more afflicted by obesity than the United States are Middle Eastern countries like Saudi Arabia and Kuwait. A large chunk of their drinking water comes from the ocean, consistently high in lithium.
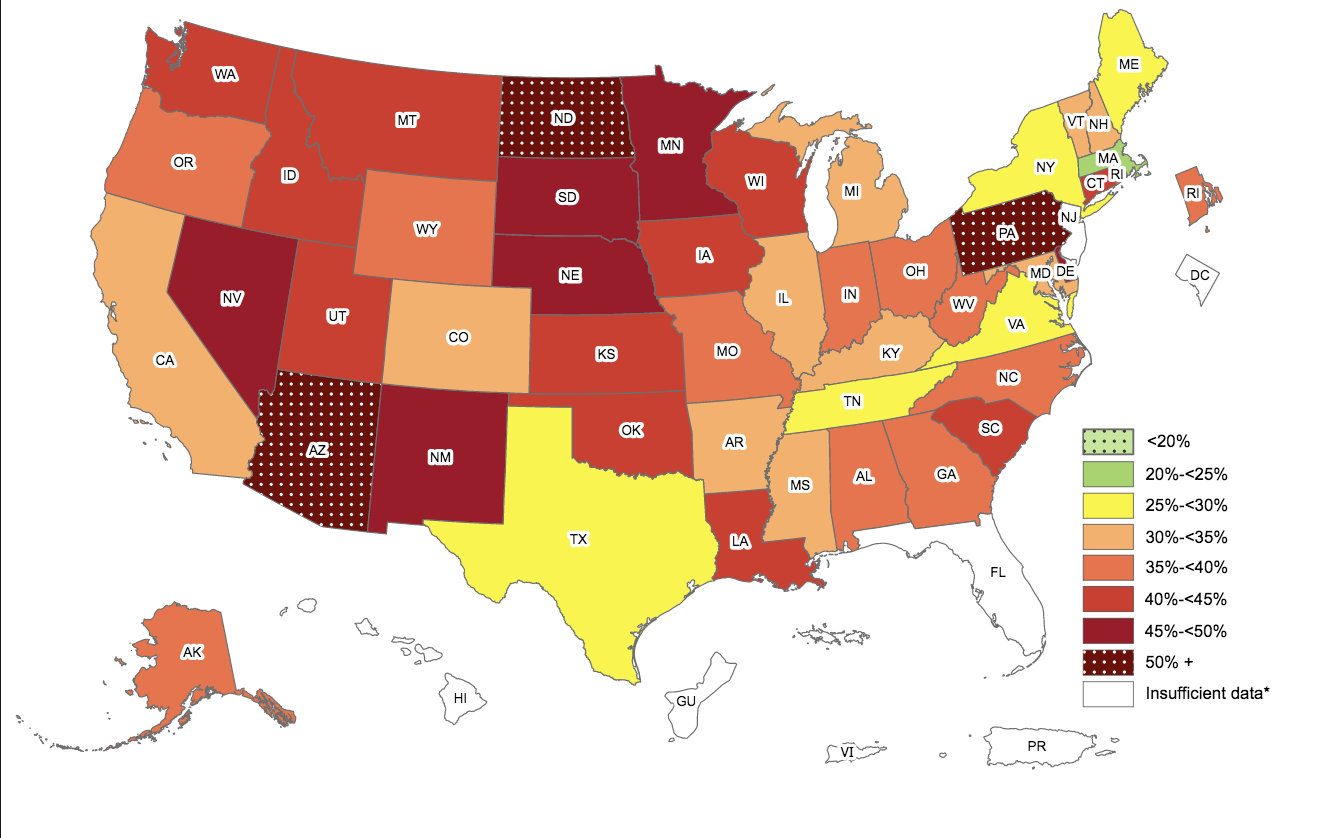
Interestingly, a county-wide map reveals a clear trend: the Appalachian and Rocky Mountains are notably lean and the Mississippi River basin is notably obese. A chemical pollutant would be less common in areas with higher elevation and increase in dosage as it travels through waterways.
Obesity in the United States by county [16]
A third contender is seed and vegetable oils; specifically canola, corn, rapeseed, grapeseed, sesame, soybean, peanut, and flaxseed oils. Such oils are made of poly-unsaturated fatty acids, or PUFAs. During processing, transport, and cooking, these oils are exposed to high heats which cause them to break down and oxidize. Fats break down into free radicals that desperately try to react with other molecules. These radicals damage cells and cause inflammation in many parts of the body. Inflammation doesn’t sound like a big deal, but doctors have linked it to almost every modern disease: cardiovascular disease, diabetes, obesity, cancer, asthma, autoimmune disease, and psychiatric disorders [24]. These diseases are all but nonexistent in pre-industrial populations. Israel is a case study with one of the highest ratios of polyunsaturated fat to other fats, and unsurprisingly Israel is on par with the United States in obesity, cancer, hypertension, and cardiovascular disease [26].
Soybean oil production line [27]
Seed oils are a recent but pervasive phenomenon. A hundred years ago, Americans cooked using mostly butter, olive oil, lard, beef tallow, or other animal fats. Food companies only introduced seed oils in the 1960s and 1970s, and their consumption has skyrocketed ever since as a cheaper alternative to animal fats[28]. Over the course of just the twentieth century, the average American went from eating 0.009 to 11.64 kilograms of soybean oil per year – an astronomical increase [29]. These oils now compose 20% of our caloric intake. These fats are so pervasive that I find it difficult to find a processed food that does not contain one of these oils.
Seed oils, like antibiotic runoff and lithium, are all relatively new, pervasive throughout the United States, and invisible to everyday people.
A growing movement seeks to normalize obesity, and many Americans grew up in a country where obesity is widespread and expected. If you are of a healthy weight, it’s easy to believe obesity comes from diet and exercise, and with effort and self-control you have achieved what many could not. If you are obese, it’s easy to believe that genetics are at fault, and you happen to be predisposed to obesity. These mindsets shrug the burden of responsibility from our government and corporations to individuals or pure random chance. Our society cannot solve the problem if we don’t understand it, and I want to convince you that obesity is a social problem with systemic solutions.
A few years ago, as mayor of New York City, Michael Bloomberg famously attempted to ban sugary beverages larger than 16 ounces at food-service establishments in the city. This ban excluded supermarkets, vending machines, and convenience stores and still allowed refills. In other words, anyone who wanted a soda could still get it, but the beverage industry still took legal action against the city, and a Manhattan judge struck it down. Even a toothless, trivial law in the right direction faces blowback by the business interests it hurts.
Seed oil consumption did not spike due to independent choices by consumers, but top-down government and corporate policies. In 1911, Proctor and Gamble pioneered the industrial process to produce seed oils, specifically a cooking fat alternative Crisco, and has marketed them as healthier than saturated fat ever since. In 1961, the American Heart Association advised Americans to replace their saturated fats – lard, butter, tallow – with polyunsaturated fats [30]. Again in 1977, the Senate Select Committee on Nutrition and Human Needs recommended Americans to consume fewer saturated animal fats, the kind that have been consumed for all of human history [31]. The Department of Agriculture has regularly been issuing similar recommendations, and every time, the Department must compromise with the industries of different food groups and their armies of lobbyists [32].
Lithium pollution also stems from top-down forces. Rechargeable batteries, chiefly those in mobile phones, laptops, electric cars, and generators, depend highly on lithium, and as a consequence lithium production has skyrocketed in recent decades. The government has contributed: President Biden has signed an executive order aiming to make half of cars sold in the United States electric, inciting huge demand for lithium batteries. We do not even have EPA standards for lithium in drinking water, and our National Center for Health Statistics tracks a slew of minerals in our bodies, but not lithium [34].
Thankfully, the Food and Drug Administration has taken steps to curb the use of antibiotics. In 2017, the FDA banned over-the-counter antibiotics used as feed supplements for livestock [35]. Over the past few decades, the FDA has issued many guidelines for antibiotics and incentives for alternatives, and use has decreased over that time [36]. This shows that top-down government efforts can help as well as hurt.
In the largest attempt to address childhood obesity in the US in recent memory, Barack and Michelle Obama launched the Healthy and Hunger-Free Kids act of 2010, improving access to school lunches and altering nutrition standards. According to a Harvard study, overall the 30 million children affected are eating more fruits and vegetables and not wasting food in significant amounts despite such criticisms from opponents. Still, childhood obesity has only continued to increase, and the USDA under Trump has loosened the standards to the delight of food companies.
Any policy solution to tackle a problem as all-encompassing as obesity must be widespread. Past examples show that a policy of any scope, from a ban on certain sodas to a national reorganization of school lunches, necessarily has to hurt the bottom line of the companies contributing to obesity, and will necessarily face backlash. Any such policy needs to tread the fine line between being ineffective and being overbearing and unsolicited. I believe that if more people understood that industrialization and pollution of our food is overbearing and unsolicited, they would welcome widespread government measures and feel empowered to address it themselves.
Why does nutrition have to be so confusing? It’s clear that obesity stems not from personal or genetic failures, but top-down political and corporate influences. Obesity therefore has top-down political and corporate solutions. First and foremost, money in politics in the form of corporate lobbyists and Citizens United must be stamped out, and those in charge of dietary recommendations and laws must prioritize the average American’s health instead of food industry profits. The government must take steps to regulate the sale of seed oils at the expense of corporations like Procter and Gamble, as well as curb false advertisements championing the health benefits of a product. These ads display a clear conflict of interest and take a human toll.
The United States also needs to both track and regulate pollution of drinking water and human tissue. The sheer absence of information for lithium and antibiotics is devastating. Even if obesity is not directly caused by any of the sources argued for in this article, increasing our monitoring will only help reveal the true source of obesity, as well as all other problems caused by pollution. Efforts to limit climate change have emphasized electric vehicles and artificial foods over meat. While climate change presents an impending threat, we must ensure that our solutions do not cause problems of their own. Our government and corporations leading this transition must think ahead and anticipate the problems of lithium exposure and highly-processed food.
It may be that nothing in this article causes obesity. The problem goes beyond lithium, seed oils, and antibiotics. The problem is that the United States and the entire industrialized world is so careless and apathetic about new and synthetic chemicals pervading in our environment and our body. Even if every single synthetic chemical ever produced is nontoxic, their interaction with our bodies, the environment, or other synthetic chemicals can have dangerous effects. The effects of synthetic chemicals are truly outside of our control and understanding.
If we can shake the addictive and profitable stranglehold of the tobacco and nicotine industries, we can do the same with obesity. If we can acknowledge that obesity is a systemic issue with our government and corporations rather than simply diet and genetics, we can make sure our children grow up happy, healthy, and informed of what they eat.
Sources
1. Gonzalez, Alina Polyakova and Geysha. “Why the U.S. Anti-Smoking Campaign Is a Great Model for Fighting Disinformation.” Brookings (blog), August 7, 2018. https://www.brookings.edu/blog/order-from-chaos/2018/08/07/why-the-u-s-anti-smoking-campaign-is-a-great-model-for-fighting-disinformation/.
2. Desliver, Drew. “How America’s Diet Has Changed over Time.” Pew Research Center (blog). Accessed December 28, 2021. https://www.pewresearch.org/fact-tank/2016/12/13/whats-on-your-table-how-americas-diet-has-changed-over-the-decades/.
3. Schiller, Jeannine S. “National Health Interview Survey Early Release Program,” 2017, 123.
4. Pomeroy, Ross. “The Prison Study That Changed How Scientists View Obesity | RealClearScience.” Accessed December 28, 2021. https://www.realclearscience.com/blog/2019/11/02/the_prison_study_that_changed_how_scientists_view_obesity.html.
5. Landsverk, Gabby. “Americans Are Eating Less Sugar, More Sweeteners but Aren’t Healthier,” July 28, 2020. https://www.insider.com/americans-are-eating-less-sugar-more-sweeteners-but-arent-healthier-2020-7.
6. Marlowe, Frank W., J. Colette Berbesque, Brian Wood, Alyssa Crittenden, Claire Porter, and Audax Mabulla. “Honey, Hadza, Hunter-Gatherers, and Human Evolution.” Journal of Human Evolution 71 (June 2014): 119–28. https://doi.org/10.1016/j.jhevol.2014.03.006.
7. Ichikawa, Mitsuo. “ECOLOGICAL AND SOCIOLOGICAL IMPORTANCE OF HONEY TO THE MBUTI NET HUNTERS, EASTERN ZAIRE,” n.d., 14.
8. Lindeberg, S., E. Berntorp, P. Nilsson-Ehle, A. Terént, and B. Vessby. “Age Relations of Cardiovascular Risk Factors in a Traditional Melanesian Society: The Kitava Study.” The American Journal of Clinical Nutrition 66, no. 4 (October 1997): 845–52. https://doi.org/10.1093/ajcn/66.4.845.
9. Tobias, Deirdre K., Mu Chen, JoAnn E. Manson, David S. Ludwig, Walter Willett, and Frank B. Hu. “Effect of Low-Fat Diet Interventions versus Other Diet Interventions on Long-Term Weight Change in Adults: A Systematic Review and Meta-Analysis.” The Lancet Diabetes & Endocrinology 3, no. 12 (December 1, 2015): 968–79. https://doi.org/10.1016/S2213-8587(15)00367-8; Heini, A. F., and R. L. Weinsier. “Divergent Trends in Obesity and Fat Intake Patterns: The American Paradox.” The American Journal of Medicine 102, no. 3 (March 1997): 259–64. https://doi.org/10.1016/S0002-9343(96)00456-1.
10. McDougall, John. “Extreme Nutrition: The Diet of Eskimos*.” Forks Over Knives, October 5, 2015. https://www.forksoverknives.com/wellness/extreme-nutrition-the-diet-of-eskimos/.
11. Petersen, Irene Berg. “The Maasai keep healthy despite a high-fat diet,” September 11, 2012. https://sciencenordic.com/denmark-diseases-exercise/the-maasai-keep-healthy-despite-a-high-fat-diet/1376530.
12. Bartoshuk, Linda. “Learning to Like Foods.” APS Observer 23 (March 1, 2010). https://www.psychologicalscience.org/observer/learning-to-like-foods.
13. Sampey, Brante P., Amanda M. Vanhoose, Helena M. Winfield, Alex J. Freemerman, Michael J. Muehlbauer, Patrick T. Fueger, Christopher B. Newgard, and Liza Makowski. “Cafeteria Diet Is a Robust Model of Human Metabolic Syndrome With Liver and Adipose Inflammation: Comparison to High-Fat Diet.” Obesity 19, no. 6 (2011): 1109–17. https://doi.org/10.1038/oby.2011.18.
14. Elks, Cathy. “Frontiers | Variability in the Heritability of Body Mass Index: A Systematic Review and Meta-Regression | Endocrinology.” Accessed December 28, 2021. https://www.frontiersin.org/articles/10.3389/fendo.2012.00029/full.
15. Herrera BM, Keildson S, Lindgren CM. Genetics and epigenetics of obesity. Maturitas. 2011;69(1):41-49. doi:10.1016/j.maturitas.2011.02.018
16. “American Obesity Treatment Association - Obesity in America.” Accessed December 28, 2021. https://www.americanobesity.org/obesityInAmerica.htm.
17. Riley, Lee, Eva Raphael, and Eduardo Faerstein. “Obesity in the United States – Dysbiosis from Exposure to Low-Dose Antibiotics?” Frontiers in Public Health 1 (2013): 69. https://doi.org/10.3389/fpubh.2013.00069.
18. Kirchhelle, Claas. “Pharming Animals: A Global History of Antibiotics in Food Production (1935–2017) | Humanities and Social Sciences Communications.” Accessed December 28, 2021. https://www.nature.com/articles/s41599-018-0152-2.
19. Turner-McGrievy, Gabrielle, Trisha Mandes, and Anthony Crimarco. “A Plant-Based Diet for Overweight and Obesity Prevention and Treatment.” Journal of Geriatric Cardiology : JGC 14, no. 5 (May 2017): 369–74. https://doi.org/10.11909/j.issn.1671-5411.2017.05.002.
20. Amdisen, Amdi. “Serum Level Monitoring and Clinical Pharmacokinetics of Lithium.” Clinical Pharmacokinetics 2, no. 2 (April 1, 1977): 73–92. https://doi.org/10.2165/00003088-197702020-00001.
21. U.S. Department of the Interior. “Professional Paper.” Professional Paper. Professional Paper, 2017.
22. Alsabbagh, Ahmad, Sewar Aljarrah, and Majdi Almahasneh. “Lithium Enrichment Optimization from Dead Sea End Brine by Chemical Precipitation Technique.” Minerals Engineering 170 (August 15, 2021): 107038. https://doi.org/10.1016/j.mineng.2021.107038; Abdul-Rahim, H. F., G. Holmboe-Ottesen, L. C. M. Stene, A. Husseini, R. Giacaman, J. Jervell, and E. Bjertness. “Obesity in a Rural and an Urban Palestinian West Bank Population.” International Journal of Obesity and Related Metabolic Disorders: Journal of the International Association for the Study of Obesity 27, no. 1 (January 2003): 140–46. https://doi.org/10.1038/sj.ijo.0802160; Djalalinia, Shirin, Sahar Saeedi Moghaddam, Ali Sheidaei, Nazila Rezaei, Seyed Sina Naghibi Iravani, Mitra Modirian, Hossein Zokaei, et al. “Patterns of Obesity and Overweight in the Iranian Population: Findings of STEPs 2016.” Frontiers in Endocrinology 11 (2020): 42. https://doi.org/10.3389/fendo.2020.00042; Pouraghabarar, Minoo, Mojtaba S. Taleshi, and Mohammad Javad Chaichi. “Determination of Lithium Abundances in Seawater in the Southern Coast of the Caspian Sea and River Estuaries.” Journal of Marine Science and Technology 19, no. 4 (February 19, 2021): 66–72. https://doi.org/10.22113/jmst.2018.109755.2088.
23. Department of Animal Science, Cornell University, Ithaca, NY, USA, and Ling Tao. “Oxidation of Polyunsaturated Fatty Acids and Its Impact on Food Quality and Human Health.” Advances in Food Technology and Nutritional Sciences - Open Journal 1, no. 6 (December 31, 2015): 135–42. https://doi.org/10.17140/AFTNSOJ-1-123.
24. Petrone, Andrew B, Natalie Weir, Naomi Q Hanson, Robert Glynn, Michael Y Tsai, J Michael Gaziano, and Luc Djoussé. “Omega-6 Fatty Acids and Risk of Heart Failure in the Physicians’ Health Study.” The American Journal of Clinical Nutrition 97, no. 1 (January 1, 2013): 66–71. https://doi.org/10.3945/ajcn.112.048991.
25. Wang, Lu, JoAnn E. Manson, Susanne Rautiainen, J Michael Gaziano, Julie E. Buring, Michael Y. Tsai, and Howard D. Sesso. “A Prospective Study of Erythrocyte Polyunsaturated Fatty Acid, Weight Gain, and Risk of Becoming Overweight or Obese in Middle-Aged and Older Women.” European Journal of Nutrition 55, no. 2 (March 2016): 687–97. https://doi.org/10.1007/s00394-015-0889-y; Pan, D. A., and L. H. Storlien. “Dietary Lipid Profile Is a Determinant of Tissue Phospholipid Fatty Acid Composition and Rate of Weight Gain in Rats.” The Journal of Nutrition 123, no. 3 (March 1993): 512–19. https://doi.org/10.1093/jn/123.3.512.
26. Keinan-Boker, Lital, Nitzan Noyman, Ayelet Chinich, Manfred S. Green, and Dorit Nitzan-Kaluski. “Overweight and Obesity Prevalence in Israel: Findings of the First National Health and Nutrition Survey (MABAT).” The Israel Medical Association Journal: IMAJ 7, no. 4 (April 2005): 219–23; Yam, D., A. Eliraz, and E. M. Berry. “Diet and Disease--the Israeli Paradox: Possible Dangers of a High Omega-6 Polyunsaturated Fatty Acid Diet.” Israel Journal of Medical Sciences 32, no. 11 (November 1996): 1134–43.
27. Seed Oil Press. “Soybean Oil Production Line, Soybean Oil Extraction Plant Project,” April 30, 2018. https://www.seedoilpress.com/oil-production-plant/soybean-oil-production-line.html.
28. Hope, Katie. “Obesity Crisis: Is This the Food That Is Making Us All Fat? - BBC News,” March 15, 2017. https://www.bbc.com/news/business-39254804.
29. Blasbalg, Tanya L, Joseph R Hibbeln, Christopher E Ramsden, Sharon F Majchrzak, and Robert R Rawlings. “Changes in Consumption of Omega-3 and Omega-6 Fatty Acids in the United States during the 20th Century123.” The American Journal of Clinical Nutrition 93, no. 5 (May 2011): 950–62. https://doi.org/10.3945/ajcn.110.006643.
30. Sacks, Frank M. “Dietary Fats and Cardiovascular Disease: A Presidential Advisory From the American Heart Association | Circulation,” June 15, 2017. https://www.ahajournals.org/doi/full/10.1161/CIR.0000000000000510.
31. Oppenheimer, Gerald M., and I. Daniel Benrubi. “McGovern’s Senate Select Committee on Nutrition and Human Needs Versus the: Meat Industry on the Diet-Heart Question (1976–1977).” American Journal of Public Health 104, no. 1 (January 2014): 59–69. https://doi.org/10.2105/AJPH.2013.301464.
32. “1985 Dietary Guidelines for Americans | Dietary Guidelines for Americans.” Accessed December 28, 2021. https://www.dietaryguidelines.gov/about-dietary-guidelines/previous-editions/1985-dietary-guidelines-americans; Jacoby, Richard. “The FDA’s Phony Nutrition Science: How Big Food and Agriculture Trumps Real Science -- and Why the Government Allows It | Salon.Com,” April 12, 2015. https://www.salon.com/2015/04/12/the_fdas_phony_nutrition_science_how_big_food_and_agriculture_trumps_real_science_and_why_the_government_allows_it/.
33. Nast, Condé. “The Spiralling Environmental Cost of Our Lithium Battery Addiction.” Wired UK. Accessed December 28, 2021. https://www.wired.co.uk/article/lithium-batteries-environment-impact; Rapaport, Lisa. “Lithium from Electronic Waste Can Contaminate Water Supply.” Reuters, December 18, 2019, sec. Healthcare & Pharma. https://www.reuters.com/article/us-health-water-lithium-idUSKBN1YM2JW.
34. “NHANES 2013-2014 Laboratory Data.” Accessed December 28, 2021. https://wwwn.cdc.gov/nchs/nhanes/search/datapage.aspx?Component=Laboratory&CycleBeginYear=2013; United States Environmental Protection Agency. “2018 Edition of the Drinking Water Standards and Health Advisories Tables,” March 2018. https://www.epa.gov/sites/default/files/2018-03/documents/dwtable2018.pdf.
35. AccessScience Editors. “U.S. Bans Antibiotics Use for Enhancing Growth in Livestock - AccessScience from McGraw-Hill Education,” January 2017. https://www.accessscience.com/content/BR0125171.
36. U.S. Food and Drug Administration. “Timeline of FDA Action on Antimicrobial Resistance.” FDA, May 3, 2021. https://www.fda.gov/animal-veterinary/antimicrobial-resistance/timeline-fda-action-antimicrobial-resistance; “2020 Summary Report On Antimicrobials Sold or Distributed for Use in Food-Producing Animals,” December 2021, 49.
37. Carson, Rachel, 1907-1964. Silent Spring. Boston :Houghton Mifflin, 2002.
